If you are suddenly experiencing odd things happening inside your mouth, it is completely normal to wonder why this is. Especially if you are experiencing symptoms that are inhibiting your ability to eat or interrupting your daily routine. The next thing you may wonder is whether or not you’re going to need a root canal.
The fact of the matter is, there is no way to know for sure if you need a root canal without a visit to your local dentist’s office. Only your general dentist can evaluate your symptoms to accurately diagnose what type of dental treatment is best to address these symptoms. In some cases, this may call for a root canal, while in other cases it may call for another restorative treatment.
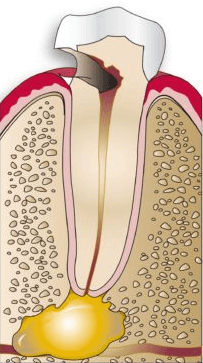
Simply stated, you will need a root canal if the dental pulp on the inside of your tooth is infected. Pulpitis, or infected dental pulp, occurs when bacteria are able to enter the inside of the tooth through severely decayed or damaged areas. Since bacteria cause the dental pulp to die and decay, the only way to prevent the spread of infection and save the tooth is to perform a root canal. During a root canal, the dead and decayed tissue will be removed from the pulp chambers and root canals. The tooth nerve will also be removed, which will alleviate possible tooth pain caused by the infection.
Although only a general dentist can diagnose a pulp infection, here are some common signs that may indicate a trip to your local dental office is needed:
Toothache
This is one of the most noticeable symptoms and it is often the symptom that causes people to question whether or not they need a root canal. Toothaches caused by pulp infections are the result of swelling inside the tooth that causes pressure on the tooth’s nerve. When caused by a pulp infection, toothaches usually come on suddenly and get progressively worse over time. An achy tooth may also be accompanied by tooth sensitivity to hot and cold temperatures, as well as sugary, sticky foods.
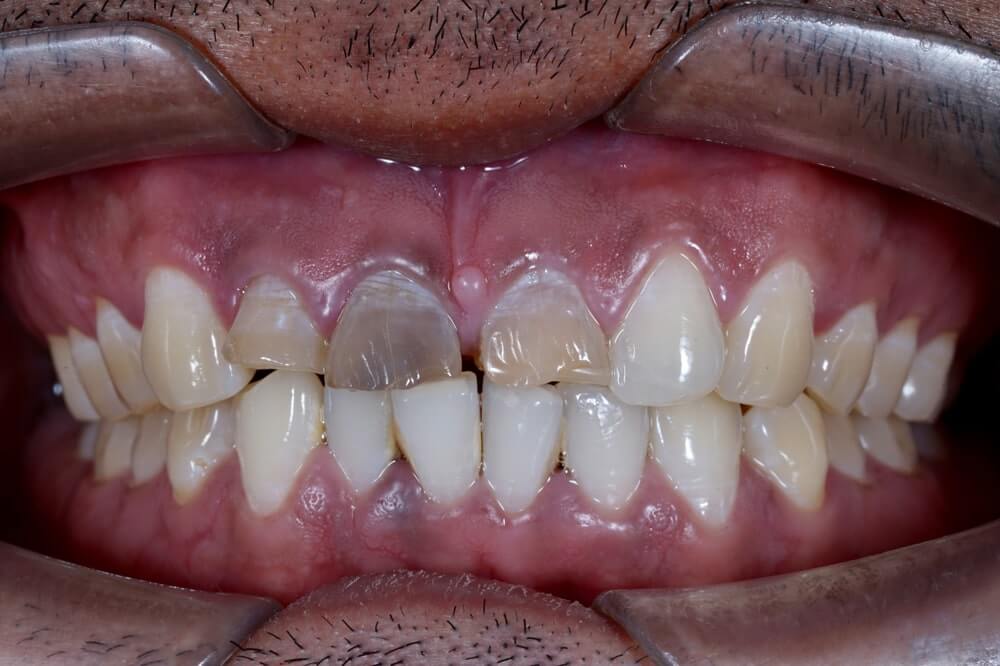
Discolored Tooth
When one tooth does not look like the others, this can indicate the need for a root canal. A single tooth may become discolored if its dental pulp is dead or dying as a result of a pulp infection. Depending on the severity of the infection and how much tissue is dead or dying, there are a range of colors to look for. Dark yellow, light gray, light brown, and black are some common discolorations associated with pulp infections.
Gum Issues
Although pulp infections primarily affect the inside of the tooth, they can also affect the gum tissue in cases where the bacteria has spread. This can cause the gums to appear red and swollen, and they will likely be tender to the touch. In some cases, pimples or abscesses may form along the gum line around the affected tooth.
Overall, if you are questioning whether or not you need a root canal, the best thing to do is schedule an appointment with your local dental office. While toothaches, a discolored tooth, and gum issues can all indicate a possible pulp infection, only a general dentist can provide an expert diagnose and treatment options. In the case of a pulp infection, a root canal will be needed to prevent further dental complications.